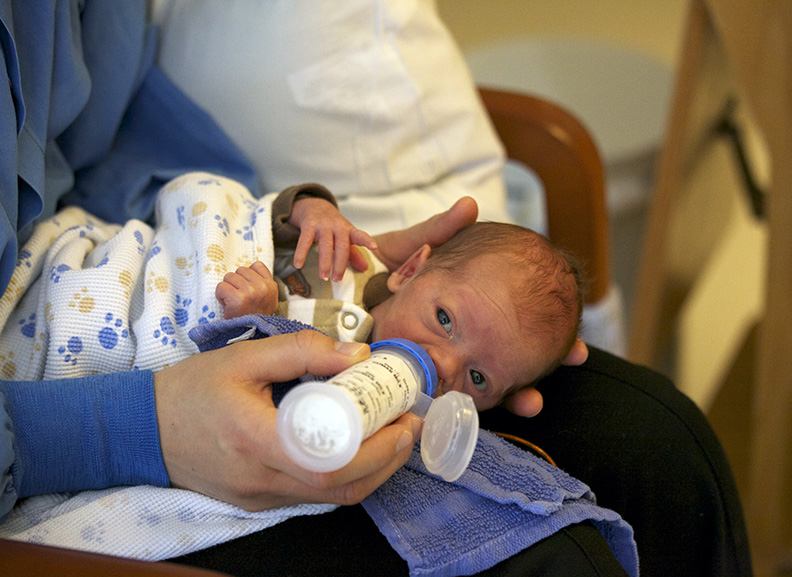
Infant Driven Feeding
I had the opportunity to listen to a CCC-SLP talk about infant driven feeding and working with infants to learn how to eat in a positive manner. I know for most of you this might seem like a simple concept, but for all babies it is an acquired skill.Please recognize that I am not a SLP, but I am a pediatric RD and I have been trained in infant feeding and the SOS feeding method. I am not here to try to diagnose swallow dysfunction, but instead to focus on watching feeding cues and helping to create a positive feeding environment.
A baby in utero starts to suck and swallow as early as 12 weeks gestation. Throughout their time in utero they are sucking in amniotic fluid and then swallowing it and peeing it out. The act of eating is a series of processes - sucking, swallowing and breathing and doing this in a coordinated manner. For those babies born early, they miss out on practicing this skill in utero. We will watch for oral feeding cues around the 32-34 week gestation mark and then often infants will be allowed to start orally feeding ~34 weeks gestation with proper feeding cues.
Well what are feeding cues? Feeding cues include behaviors that a baby is going to show that they are hungry. This could include, waking up, starting to move around/fuss, putting hands in our around their mouth, and rooting whenever anything gets near their mouth. Most of us are familiar with cues to show that a baby might be hungry.
I would say that most adults are less familiar with stress cues. What are stress cues? These are signs that a baby is showing that they don’t want to eat. This would be if they are arching/pulling away from the bottle or breast, if their brow is furrowed, if they are excessively blinking their eyes, crying, trying to not latch onto the bottle or breast, not opening their mouth, putting their tongue to the roof of their mouth or simply not sucking on the bottle or breast. These are all signs that the baby isn’t ready or wanting to orally feed.
For most term infants who are healthy, after the first few days of life they are getting the eating routine down and they learn those skills and take off. With preterm infants, this is a lot harder and they don’t tend to have such positive experiences all the time. Eating is extremely hard work, it is exhausting and if they are sick, have low stores and can easily burn more calories than they are consuming if feedings go longer than 30 minutes. Plus if you are pushing a baby to orally feed, who isn’t ready you can create a feeding problem. That baby can silently choking or aspirate that breast milk or formula and that can lead to an infection, like pneumonia. Unlike older children or adults, babies don’t really cough when they choke. They can still choke on a feeding and you wouldn’t know (we call that silent aspiration).
Why I am going through and sharing this information with you all? Because this has been a topic of discussion in our NICU, because one of the basic things a baby needs to do to go home is eat. So much focus is placed on volume intakes and growth and parents get caught up in volumes and trying to meet numerical goals. Volumes do matter, but honestly for the long term development of a child, volumes don’t matter as much as the quality of the feeding. Is the child calm, able to coordinate sucking, swallowing and breathing and are they able to take an appropriate volume in an appropriate amount of time while keeping their composure. Having well trained RNs who can watch for stress cues and are able to help teach the baby who is eat in a calm way is key to the long term feeding success for that child. Most parents who have term infants, don’t have to stress and worry about feedings in the same way as a parent of a preterm infant. The key is help teach parents how to properly feed their preterm baby so that the baby and the parents are not stressed. Whether you are feeding your preterm or term baby, make sure you watch for any stress cues with PO feedings and then stop a feeding if the baby isn’t able to maintain a calm state. It is not worth force feeding a baby. If you have questions or concern about your child and feeding, reach out to your pediatrician to talk about your concerns and they can help get you in touch with SLP to discuss any oral motor feeding concerns.